Media Releases
Review finds remote nurse safety lacking
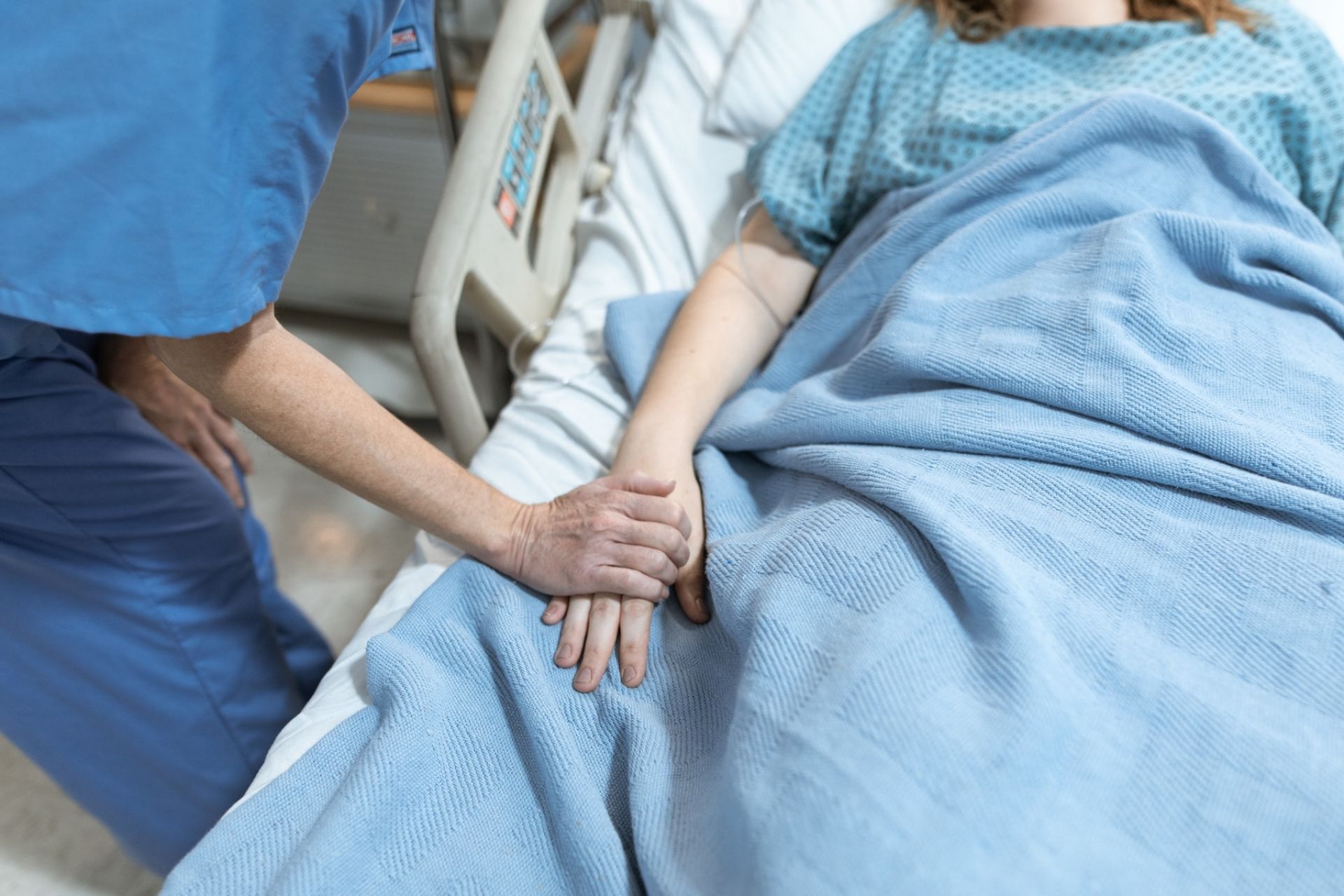
Urgent improvements are needed to ensure the safety of nurses working in remote areas, a new study has found.
Laura Wright, from James Cook University’s Murtupuni Centre for Rural and Remote Health, said her review of literature focusing on workplace safety for nurses in remote areas found many safety recommendations, going as far back as 1995, have not been implemented.
Ms Wright said the absence of adequate safety measures for Remote Area Nurses (RANs) was likely due to a lack of funding and resources.
“It’s a problem for remote health in general. It’s a really resource-poor environment, you’re trying to provide a service in extremely remote settings, and that can be expensive,” she said.
“Understaffing and high staff turnover has been a huge problem in remote health for a long time.”
RAN safety was put into the spotlight following the tragic murder of South Australian nurse Gayle Woodford in 2016.
That prompted the South Australian government to pass legislation known as “Gayle’s Law”, which made it mandatory for health practitioners working in remote areas of South Australia to be accompanied by a second responder when attending an out-of-hours or unscheduled call-out.
No other Australian state or territory had legislated similar safety measures, although some have safety guidelines for RANs.
Ms Wright said some of the more recent safety recommendations looked at what could be done with existing resources, such as requiring patients to present to the clinic after hours and not staff accommodation, having a nurse notify a colleague prior to attending urgent call-outs away from the clinic, and managers actually listening to the concerns and suggestions of their staff.
The last research measuring workplace violence towards RANs, published more than 10 years ago, found there had been a statistically significant increase in workplace violence experienced by RANs between 1995 and 2008.
Nearly 30 per cent of participants had personally experienced physical violence in the preceding 12 months.
A 2017 report published by remote health workforce body CRANAplus found 25 per cent of participating RANs still did not have safe and secure accommodation or workplaces, even though staff accommodation and clinic building safety had been discussed for decades in peer-reviewed literature.
Unsafe staff accommodation had led to some severe incidents, which was raised in that report and some news articles.
Ms Wright, a registered nurse, said while remote area nursing was an enjoyable profession that had many dedicated professionals, a collaborative approach was needed between state and territory governments, communities and other stakeholders to ensure there were adequate protections in place.
“A lot of nurses who I have interviewed since completing this scoping review say it is such a rewarding job but there is a lot more that can be done to make it safer,” she said.
“For our remote areas, we’re falling down when it comes to primary healthcare needs, so taking away some of the barriers for clinicians who are working to help address that would be really valuable.”
Ms Wright said the next stage of her research project will involve publishing the feedback from RANs she had interviewed about the effectiveness of existing safety measures in various remote communities around Australia.
Media enquiries: michael.serenc@jcu.edu.au